How to expel inflammation from the body?

In the context of the coronavirus epidemic, there is increasing information that we should reduce the intensity of inflammatory reactions in the body, because inflammation is a major contributor to life-threatening complications in this disease. However, we should fight inflammation all the time. In its chronic form, it is a condition that contributes to the development of many diseases, including the most serious ones.
Inflammation is an important mechanism that allows the body to respond quickly to damage to any tissue in the body. When we cut our finger, the area around the wound becomes slightly red and swollen over a few hours, and when we apply pressure, it hurts. This is despite the fact that no infection has entered the wound. This is because inflammation allows the healing process to proceed properly.
The same happens if the injury occurs inside the body – for example, if we break our arm or sprain our ankle. The fact that the sprain hurts much more the next day is due to inflammatory processes. While only the damaged ligaments or joint capsule hurt immediately after the injury, the next day there is also intense inflammation affecting the surrounding tissues.
Infection-related inflammation is also of the same origin – for example, viruses or bacteria damage the cells of the mucous membrane inside the throat, and in response, a painful inflammation starts in the throat.
Acute inflammation benefits, chronic inflammation harms
Acute inflammation resulting from injury or infection may hurt, but otherwise it is a clearly positive process. In the case of infections, it allows the immune system to effectively fight the causative agents, while in the case of injuries, it contributes to the removal of damaged tissue so that it can be replaced with new tissue. However, the problem arises in the case of chronic inflammation, which causes permanent tissue damage.
Athletes know this problem intimately. For example, if they overdo it with training or have imbalances in the body that lead to overloading of certain muscle parts, small microscopic injuries occur both in the muscle itself and in the structure of the tendon and its attachment. Compared to a sprain, for example, it hurts relatively little (it is an injury of an order of magnitude less), so the athlete often continues training. Not only does the inflammation not go away, but as more damage is added to the existing, unhealed damage, its intensity increases and the internal structure of the tendon changes. Over time, the inflammation grows into a chronic form that is difficult to treat and often leads to long periods of forced rest. In extreme cases, the tendon may even rupture.
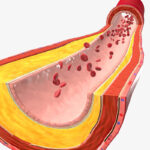
Chronic inflammation, however, can arise in virtually any place in the body. In some cases it is a complication, a consequence of a disease, but in other cases it is one of its root causes. Thus, inflammation is at the origin of atherosclerosis, as well as some cancers (such as bowel tumours) and diabetes. And in many others, it minimally worsens the course. A typical example is arthrosis. In this degenerative joint disease, although cartilage is first damaged, these processes result in inflammation, which gradually increases and then damages other joint structures. Suppressing inflammatory processes in the body is therefore a matter that will have a positive effect on the health of virtually the entire body.
Inflammation from the perspective of epigenetics
The actual development of inflammation is a very complex process. It takes place at the cellular level and is accompanied by activation or suppression of the activity of a number of genes. This happens through biochemical reactions that we call epigenetic.
The epigenetic nature is, for example, the activation of immune cells, which then not only attach to the damaged tissue, but also produce a number of inflammation-promoting substances.
Cytokines also play an important role. These are proteins whose production is on the one hand influenced by epigenetic factors (e.g. lifestyle), but on the other hand they themselves have significant epigenetic effects because they influence the activity of many other genes and participate in the so-called cell signalling, which is the process of information transfer between cells and within cells themselves. Pro-inflammatory cytokines include some interleukins (ILs) and TNF-alpha.
The enzyme cyclooxygenase 2 (COX-2) is also very important. It is essential for the production of substances called prostaglandins, which are crucial not only for the course of inflammation itself, but also for the development of fever – prostaglandin E2 in particular affects cells in the hypothalamus, which is responsible for thermoregulation.
The basis is dietary modification
Therefore, when fighting inflammation, it is important to focus on reducing the activity of pro-inflammatory genes and promoting anti-inflammatory ones. In particular, limiting the production of pro-inflammatory cytokines and the COX-2 enzyme is essential. The most effective way is mainly dietary modification.
One of the factors that most promote inflammation is a diet high in carbohydrates, especially “fast” sugars with a high glycaemic index. There are a number of studies that have confirmed this, and to increase inflammation levels, it is usually enough to add a relatively small amount of sugars to the diet – for example, the volunteers were asked to add an extra can of sweetened lemonade, 50g of white bread or 50g of fructose to their usual diet. These small changes led, for example, to an increase in CRP-protein levels, which indicates the course of inflammatory processes, an increase in LDL-cholesterol levels or the production of the inflammatory factor NF-kB.
And of course the reverse is also true – it is not necessary to eliminate carbohydrates from the diet completely, even a relatively moderate reduction in their consumption will have a positive effect.
More omega-3, less omega-6
In addition to limiting carbohydrate consumption, it is also advisable to include as many foods with anti-inflammatory properties as possible. These include in particular fruits and vegetables, olive oil, many herbs, spices, and omega-3 unsaturated fatty acids.
For omega-3s, it is important not only to have sufficient intake in absolute terms, but also to have a ratio of omega-3s to omega-6 unsaturated fatty acids. While these are essential for health, they promote inflammatory processes, so it is essential that their ratio to anti-inflammatory omega-3s is as low as possible. The optimum ratio is considered to be 3:1, with a maximum of 4:1, but the standard Western diet contains several times more. Another problem here is the excessive consumption of vegetable oils, which, although cholesterol-free, contain very little omega-3 and a lot of omega-6 unsaturated fatty acids.
Obesity is a whole-body inflammation
Another important measure is maintaining an optimal weight. Moderate overweight does not matter, but if there is a greater amount of adipose tissue in the body, immune cells penetrate it, which are subsequently activated, leading to the development of inflammatory processes. Thus, obesity essentially represents a mild body-wide inflammation that, in addition to different methylation patterns, contributes to an increased risk of a number of serious diseases.
Regular bending also has an anti-inflammatory effect.
Medication or dietary supplements?
Drugs from the category of non-steroidal antirheumatic drugs (NSAIDs), such as aspirin or ibuprofen, are often used to control inflammation and pain. The principle of their action is the suppression of COX-2 production.
Unfortunately, NSAIDs suppress not only the production of the inflammatory enzyme COX-2, but also a similar substance called COX-1. This enzyme is also involved in the production of prostaglandins, but these are prostaglandins that play an important role in protecting the lining of the stomach and duodenum. If there is not enough of them, the protection of the mucosa against the action of stomach acids does not work and it is disrupted, which can lead to life-threatening bleeding. In addition, NSAIDs increase the risk of heart attack and stroke after just one week of use (this does not apply to aspirin). They also increase the risk of inflammatory bowel disease, kidney problems and possibly erectile dysfunction.
Although there are already drugs that only suppress the production of COX-2 but not COX-1, it is good to know that similar effects can be achieved by natural means, i.e. The combination of lifestyle changes with nutrient supplementation and herbs that work on the so-called epigenetic principle – they suppress the activity of the genes that produce the COX-2 enzyme in the body, but leave the production of COX-1 unchanged or even boost it. As a result, they are both strongly anti-inflammatory and pain-relieving. Although their effect is not as immediate as swallowing a pink pill, they are an effective way to suppress not only chronic inflammation but also long-term chronic pain. In fact, research has confirmed that a number of epigenetic changes occur in the DNA of chronic pain sufferers.
Dietary supplements to relieve inflammation
Boswellia – very effectively inhibits the production of COX-2 and inflammatory cytokines. It is effective not only in fighting inflammation, but also in treating chronic pain.
Ginger – taking 500 mg of ginger extract twice a day for joint pain caused by arthritis has been shown to be as effective as taking 400 mg of ibuprofen 3 times a day. It is even effective for migraines.
Rosemary – a very effective anti-inflammatory herb is particularly effective in relieving inflammation and joint pain.
EGCG – a strong anti-inflammatory effect is also possessed by green tea extract rich in epigallocatechin gallate.
Curcumin – is one of the strongest natural anti-inflammatory substances and is therefore effective against many types of chronic pain.
Omega-3s – if taken as a supplement in addition to foods containing them, this will help improve their ratio with omega-6 unsaturated fatty acids.
Baikal coneflower – also has significant anti-inflammatory and pain-relieving effects.
- Dannenberg AJ et al. The role of COX-2 in breast and cervical cancer. Prog Exp Tum Res. 2003;37:90-106.
- P Merry, P G Winyard, C J Morris, M Grootveld, and D R Blake. Oxygen free radicals, inflammation, and synovitis: and synovitis: the current status. Ann Rheum Dis. 1989 Oct; 48(10): 864–870.
- Rostom A, Dube C, Wells G, Tugwell P, Welch V, Jolicoeur E, McGowan J (2002). „Prevention of NSAID-induced gastroduodenal ulcers“. Cochrane Database Syst Rev (4): CD002296.
- Giannina Descalzi, Daigo Ikegami,Toshikazu Ushijima, Eric Nestler, Venetia Zachariou,and Minoru Narita. Epigenetic Mechanisms of Chronic Pain. Trends Neurosci. 2015 Apr; 38(4): 237–246.
- Abdel-Tawab M, Werz O, Schubert-Zsilavecz M. Boswellia serrata: an overall assessment of in vitro, preclinical, pharmacokinetic and clinical data. Clin Pharmacokinet. 2011 Jun;50(6):349-69.
- Shan Hu, Yu Chen, Zhi-Fu Wang, Qi-Liang Mao-Ying, Wen-Li Mi, Jian-Wei Jiang, Gen-Cheng Wu, and Yan-Qing Wang ,The Analgesic and Antineuroinflammatory Effect of Baicalein in Cancer-Induced Bone Pain. https://www.hindawi.com/journals/ecam/2015/973524/
- Bharat B. Aggarwal and Kuzhuvelil B. Harikumar. Potential Therapeutic Effects of Curcumin, the Anti-inflammatory Agent, Against Neurodegenerative, Cardiovascular, Pulmonary, Metabolic, Autoimmune and Neoplastic Diseases. Int J Biochem Cell Biol. 2009; 41(1): 40–59.
- Maghbooli M, Golipour F, Moghimi Esfandabadi A, Yousefi M.Comparison between the efficacy of ginger and sumatriptan in the ablative treatment of the common migraine. Phytother Res. 2014 Mar;28(3):412-5.
- Xiang Zhang and Shuk-Mei Ho. Epigenetics meets endokrinology. J Mol Endocrinol. Author manuscript; available in PMC 2014 Jun 26.
- Menon VP, Sudheer AR. Antioxidant and anti-inflammatory properties of curcumin. Adv Exp Med Biol. 2007;595:105-25.
- Kristen Gaus, Yue Huang, Dawn A. Israel, Susan L. Pendland, Bolanle A. Adeniyi, and Gail B. Mahady. Standardized ginger (Zingiber officinale) extract reduces bacterial load and suppresses acute and chronic inflammation in Mongolian gerbils infected with cagA+Helicobacter pylori. Pharm Biol. 2009 ; 47(1): 92–98.
- Moon D.O, Kim M.O, Lee J.D, Choi Y.H, Kim G.Y. Rosmarinic acid sensitizes cell death through suppression of TNF-alpha-induced NF-kappaB activation and ROS generation in human leukemiaU937 cells. Cancer Lett. 2010;288:183–91.
- M R Al-Sereitia, K M Abu-Amerb & P Sena. Pharmacology of rosemary (Rosmarinus officinalis Linn.) and its therapeutic potentials. Indian Journal of Experimental Biology
- Vol. 37, February 1999, pp.124-131