Lyme disease: how to relieve symptoms in a natural way

In the beginning, there was a tick. Or some other insect, it’s hard to say. Maybe a characteristic spot appeared on the skin, or maybe not. Maybe the doctor diagnosed you with Lyme disease and prescribed antibiotics, maybe not. Either way, you have it now – chronic. And no one knows what to do about it.
Lyme disease belongs to diseases transmitted mainly by ticks. Its most common agent in the Americas, Borrelia burgdorferi, was discovered in 1982, but its symptoms, including its association with tick-borne transmission, were described as early as the late 19th century. In Europe, the most common causative agents are Borrelia garinii and Borrelia afzelii. Approximately 4 000 people are infected in the Czech Republic each year.
Manifestations and complications of Lyme disease
The bacteria that cause Lyme disease are spirochetes – microbes with a long spiral shape whose surface proteins are constantly changing, making it difficult for the immune system to recognise them. In addition, they are protected by a protective biofilm. The chances of the body dealing with the infection on its own are thus very low, and treatment with antibiotics is usually necessary. However, the immune system’s response varies from person to person and depends on their particular genetic make-up.
The fundamental problem, however, is diagnosis. The typical manifestations of the acute phase, i.e. the formation of a red spot with a white centre around the bite site, possibly also fever and fatigue, appear in only a fraction of persons. About 40 % of those infected do not have these symptoms and the disease progresses directly to the second phase. The first phase of the disease starts about 12 weeks after the tick attaches and is characterised by pain and swelling in the joints and muscles, but also by nerve palsy and inflammation of the heart muscle.
The above-mentioned difficulties usually subside within three months at the latest, only to develop a third phase months to years later. This stage most often involves inflammatory involvement of the skin, joints, brain and spinal cord, heart and eyes.
When treatment fails
However, a complete cure sometimes does not occur even if antibiotic treatment is started in time. It is not uncommon for people to complain of symptoms such as “brain fog” and various other cognitive problems, joint and muscle pain, fatigue, etc., even after the treatment has ended. However, their blood tests are already fine at this point. Professionally, this condition is abbreviated as PTLD (Post Treatment Lyme Disease) or is called “chronic Lyme disease”. The number of people affected is very high: 10-20% of those who are treated for Lyme disease. People who have repeated bouts of Lyme disease are at greater risk of developing it.
Why is it that in some cases the cure of Lyme disease does not occur? There may be several reasons:
- The inability of some antibiotics to disrupt the protective biofilm of bacteria.
- The fact that bacteria are capable of causing inflammation even when they are already dead.
- Recent research has shown that even fragments of bacteria can stimulate a stronger immune response in the brain than live bacteria.
It must be said that many of the symptoms of chronic Lyme disease can also be caused by live bacteria. The spirochetes are generally very small and therefore easily penetrate not only, for example, the joints, but are also able to cross the blood-brain barrier and reach the brain tissue. Very often, however, it is the dead fragments of bacteria that cause the subsequent difficulties, which is why repeated use of antibiotics has no effect in these cases
A bacterium that changes genes
Moreover, recent findings suggest that chronic Lyme disease has a strong epigenetic background. In the genome of affected people, scientists have discovered a total of 35 genes that are overexpressed (i.e. their activity is significantly higher than it should be). Most of these genes promote inflammatory processes in the body. People with chronic Lyme disease, for example, have higher levels of certain inflammatory cytokines (such as IL-1ß and IL-8).
In addition, some of these genes are also linked to epilepsy, which could explain why Lyme disease causes neurological symptoms.
Formation of blood clots
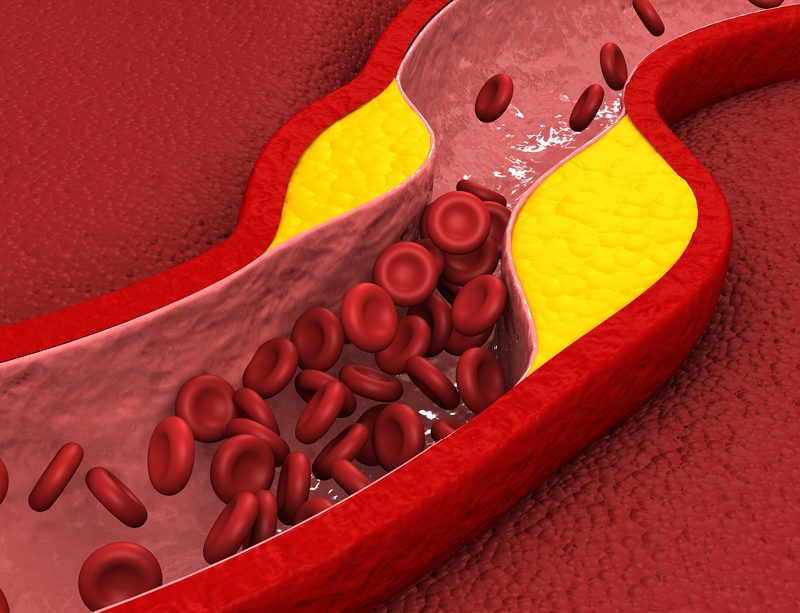
Another route by which Lyme disease infection probably produces some chronic symptoms is through the formation of blood clots or hypercoagulation. This is a common complication of many viral and bacterial infections (it is also typical of the COVID-19 virus, for example). In one study, for example, researchers found markers of low-level coagulation in 80% of Lyme disease patients. Another study found significantly higher blood concentrations of fibrinogen – the protein that makes fibrin, which subsequently forms blood clots – in 67% of infected patients. This significantly impairs the patency of small blood capillaries and causes impaired tissue oxygenation.
Effect on the hormonal system and gut microbiome
Lyme disease infection can also adversely affect the activity of certain endocrine glands. For example, thyroid function is often reduced, which is reflected, among other things, in increased fatigue and impaired immunity. The antigenic properties of Borrelia proteins are very similar to those of certain proteins associated with thyroid function, which can cause autoimmune inflammation of this organ.
Lyme disease is also often characterised by adrenal exhaustion, which in turn results in reduced corticosteroid production and therefore lower resistance to inflammatory processes. Women may also experience reduced oestrogen production, so that they sometimes experience menopause-like symptoms (e.g. hot flushes).
Moreover, the symptoms of chronic Lyme disease are very similar to those experienced by patients with a severely disrupted gut microbiome, leading scientists to think that Lyme disease could also be causing a disruption in the balance of the gut microbiome. And research has indeed confirmed this hypothesis. The change in the composition of gut bacteria is even characteristic enough that it could be used to diagnose Lyme disease in the future.
What can help?
The main problem in chronic Lyme disease is the high level of inflammatory processes, so it is important to focus on their suppression. Focusing on reducing blood clots can also help.
Dietary modification is very important, especially a significant reduction of pro-inflammatory foods (simple sugars, white flour, food additives, animal fats, soy and corn oil…) and the addition of anti-inflammatory ones, such as fruits and vegetables, quality green tea, olive oil, natural sources of omega-3 unsaturated fatty acids, fermented foods, etc. Supporting the balance of the gut microbiome should also be key, particularly through adequate consumption of soluble and insoluble fibre and fermented foods.
It is also important to focus on sleep hygiene. Sleep deprivation promotes the course of inflammatory processes, and sleep is often disturbed in Lyme disease patients.
Certain nutrients and herbs taken in the form of dietary supplements can be of significant help.
Japanese knotweed (resveratrol)
The herb, native to Northeast Asia, exhibits high antibacterial activity against the causative agents of Lyme disease. In addition, it has a strong anti-inflammatory effect. One of the reasons for this is probably the high content of resveratrol (chickweed is often used as a basis for the production of dietary supplements with resveratrol). In fact, resveratrol has a strong anti-inflammatory and neuroprotective effect (i.e. it protects nerve cells from damage), could be useful against cardiovascular symptoms of Lyme disease and has also been shown to be active against spirochetes.
Baikal pine cone
This plant, also popular especially in traditional Chinese medicine, has a strong anti-inflammatory and neuroprotective effect against Borrelia bacteria. Its great advantage is that it disrupts the protective biofilm that contributes to the bacteria’s resistance to antibiotic treatment. It is therefore highly recommended to combine it with antibiotics in the treatment of Lyme disease. In chronic Lyme disease, it is particularly useful for neurological symptoms, but it can also alleviate inflammation in the joints.
Nattokinase
An enzyme that is naturally present in the Japanese soy dish natto excels in its ability to dissolve blood clots. Therefore, it may be effective in combating hypercoagulability in Lyme disease patients. At the same time, it can help to disrupt the biofilm that protects bacteria against the immune system and antibiotic treatment (the enzyme serrapeptase has a similar effect, but its sale is currently not allowed in the Czech Republic). It is therefore also advisable to use it together with antibiotics.
Cryptolepis
The plant, native to West Africa (lat. Cryptolepis sanquinolenta), is used in local natural medicine, for example, for malaria or tuberculosis, but some studies have also confirmed a strong effect against the causative agents of Lyme disease.
Cat’s Claw
Another herb often used in the treatment of Lyme disease (Unicaria tomentosa). It has anti-inflammatory and neuroprotective effects, and some studies have confirmed its antibacterial action against the causative agent of Lyme disease. It also promotes DNA repair.
Vitamin D3
Some research suggests that Lyme disease might cause a kind of “vitamin D3 resistance”. Specifically, the infection could block the interaction between vitamin D3 and the relevant cellular receptors, and therefore infected people might need significantly more of this essential nutrient to ensure optimal body processes. A deficiency could then contribute to the development of some Lyme-related problems, such as joint inflammation. However, further research is still needed to confirm this.
Magnesium
Magnesium is another nutrient whose levels tend to be reduced in Lyme disease patients, which can also contribute to a number of problems. Supplementation is therefore advisable.
Iodine
This mineral helps to disrupt the protective biofilm of Borrelia bacteria. During treatment, it is therefore important to include sufficient sources of it in the diet.
Ginkgo biloba
Although this plant does not act against the causative agent of Lyme disease, it can significantly promote blood flow to tissues, including the brain, and has a neuroprotective effect, and is therefore particularly effective for the neurological symptoms of chronic Lyme disease.
Curcumin
Thanks to its strong anti-inflammatory effects, it can reduce inflammation and joint pain in chronic Lyme disease. It can also help to suppress inflammatory processes in the brain, thus removing ‘brain fog’, reduce the incidence of cardiac arrhythmias and suppress thyroid inflammation. However, it should not be taken during the acute phase of Lyme disease as it may reduce the effectiveness of the body’s immune response.
EGCG
Like resveratrol mentioned above, epigallocatechin gallate from green tea belongs to the so-called sirtuin activators, which are enzymes that support mitochondrial function. Among other things, it can help reduce inflammation in the brain and spinal cord.
Omega-3
Their use helps to improve cognitive function in chronic Lyme disease.
Astaxanthin
This carotenoid, which occurs naturally, for example, in salmon or shrimp, does not have a direct antibacterial effect against the causative agent of Lyme disease, but it is excellent for its anti-inflammatory and neuroprotective action, and is able to cross the blood-brain barrier and act directly in the brain tissue. Therefore, it may be effective in the neurological sequelae of Lyme disease.
Probiotics
Due to the negative impact of the disease on the balance of the gut microbiome, the use of probiotics may be effective in Lyme disease.
- Emily Henderson, B.Sc. Researchers identify 35 genes that are highly expressed in patients with long-term Lyme disease. News Medical Life Sciences. Nov 15 2022. https://www.news-medical.net/news/20221115/Researchers-identify-35-genes-that-are-highly-expressed-in-patients-with-long-term-Lyme-disease.aspx
- https://www.kliste.cz/cz/vse-o-klistatech/clanek/lymeska-borelioza
- Willis, M.D., et al. (2022) Gene set predictor for post-treatment Lyme disease. Cell Reports Medicine. doi.org/10.1016/j.xcrm.2022.100816.
- George Chaconas , Mildred Castellanos, Theodore B Verhey. Changing of the guard: How the Lyme disease spirochete subverts the host immune response. J Biol Chem. 2020 Jan 10;295(2):301-313.
- Alison W. Rebman, Kathlee Ti. Bechtold, Ting Yang, Erica A. Mihm, Mark J. Solosk, Cheryl B Novak, John N. Aucott. The Clinical, Symptom and Quality-of-Life Characterization of Well-Defined Group of Patients with Posttreatmint Lyme Disease Syndrome. Front. Med., 14 December 2017.
- U Ljøstad, A Mygland. Remaining complaints 1 year after treatment for acute Lyme neuroborreliosis; frequency, pattern and risk factors. Eur J Neurol. 2010 Jan;17(1):118-23.
- Monica E. Embers ,Stephen W. Barthold, Juan T. Borda, Lisa Bowers, Lara Doyle, Emir Hodzic, Mary B. Jacobs, Nicole R. Hasenkampf, Dale S. Martin, Sukanya Narasimhan, Kathrine M. Phillippi-Falkenstein, Jeanette E. Purcell, Marion S. Ratterree, Mario T. Philipp. Persistence of Borrelia burgdorferi in Rhesus Macaques following Antibiotic Treatment of Disseminated Infection. Plos One, January 11, 2012
- Jie Feng, Megan Weitner , Wanliang Shi, Shuo Zhang, Ying Zhang. Eradication of Biofilm-Like Microcolony Structures of Borrelia burgdorferi by Daunomycin and Daptomycin but not Mitomycin C in Combination with Doxycycline and Cefuroxime. Front Microbiol. 2016 Feb 10;7:62.
- Geetha Parthasarathy, Shiva Kumar Goud Gadila. Neuropathogenicity of non-viable Borrelia burgdorferi ex vivo. Sci Rep. 2022 Jan 13;12(1):688.
- https://drtoddmaderis.com/hypercoagulation-in-lyme-disease
- Jie Feng, Jacob Leone, Sunjya Schweig, Ying Zhang. Evaluation of Natural and Botanical Medicines for Activity Against Growing and Non-growing Forms of B. burgdorferi. Front Med (Lausanne). 2020 Feb 21;7:6.
- https://idsa.confex.com/idsa/2003/webprogram/Paper18421.html
- Goc, Anna & Niedzwiecki, Aleksandra & Rath, Matthias. Cooperation of Doxycycline with Phytochemicals and Micronutrients Against Active and Persistent Forms of Borrelia sp. Int J Biol Sci. 2016 Jul 22.
- https://aspire.care/featured/lyme-disease-herbal-treatments/
- https://www.rxlist.com/ginkgo/supplements.htm
- https://www.newnaturalsonline.com/turmeric_and_lyme.html
- Victoria Cairns. Supporting patients with long-term problems after Lyme disease. BJGP Open. 2020 Aug; 4(3): bjgpopen20X101102.
- Sunjya Schweig. Haw to Manage Inflammation in Lyme Disease. California Center for Functional Medicine. https://www.ccfmed.com/blog/manage-inflammation-in-lyme-disease
- Christian Galasso, Ida Orefice, Paola Pellone, Paola Cirino, Roberta Miele, Adrianna Ianora, Christophe Brunet, and Clementina Sansone. On the Neuroprotective Role of Astaxanthin: New Perspectives? Mar Drugs. 2018 Aug; 16(8): 247.
- Dirk Lemke a kol. Vitamin D Resistance as a Possible Cause of Autoimmune Diseases: A Hypothesis Confirmed by a Therapeutic High-Dose Vitamin D Protocol. Front. Immunol., 07 April 2021 https://www.ascent2health.com/blog/vitamin-d-and-lyme-disease
- https://heartofwellness.org/lyme-disease-may-decrease-magnesium-an-essential-mineral/
- HOW DOES LYME DISEASE AFFECT YOUR HORMONES? TORONTO FUNCTIONAL MEDICINE CENTRE, NOVEMBER 9 2020. https://torontofunctionalmedicine.com/lyme-disease-treatment/hormones/
- Nyembezi Dhliwayo, M.D, Rana Wajahat, M.D, Andriy Havrylyan, M.D, Alvia Moid, DO, Walid Khayr, M.D, and Charles P Barsano, FACE, MD, PhD. Lyme Disease: An Autoimmunity-Based “Destructive Thyroiditis” or Just Another “Non-Thyroidal Illness”? J Endocr Soc. 2021 May 3; 5(Suppl 1): A940–A941.
- Madeleine Morrissette , Norman Pitt, Antonio González, Philip Strandwitz Mariaelena Caboni, Alison W Rebman, Rob Knight, Anthony D’Onofrio, John N Aucott , Mark J Soloski, Kim Lewis. A Distinct Microbiome Signature in Posttreatment Lyme Disease Patients. mBio. 2020 Sep 29;11(5):e02310-20
- Margaret G. Gasta, MS, RDN, Christy B. Williamson, MS, CNS, Crystal M. Gossard, MS, CNS, Jessica M. Pizano, MS, CNS, Cathleen M. Burns, MS, RD, LDN, Keren E. Dolan, MS, Heather J. Finley, MS, RD, LD, CEDRD, Emily C. Parker, MS, RD, and Elizabeth A. Lipski, PhD, CNS, CCN, BCHN, IFMCP. Probiotics and Disease: A Comprehensive Summary—Part 4, Infectious Diseases. Integr Med (Encinitas). 2017 Apr; 16(2): 28–38.
- https://www.treatlyme.net/guide/lyme-disease-biofilms